...continued from {Part One}.
Sam spent two wonderful, memory-filled months at home with us. The girls didn't waste any time falling in love with him. Emory and Harper wanted to help me with everything to do with Sam, but it was especially hard to peel Emory off of him. We spent our days taking care of Sam, holding him, and taking walks around the neighborhood. We took him to church twice, I took him to MOPs twice, and he made road trips to Bertram twice.
Sam spent two wonderful, memory-filled months at home with us. The girls didn't waste any time falling in love with him. Emory and Harper wanted to help me with everything to do with Sam, but it was especially hard to peel Emory off of him. We spent our days taking care of Sam, holding him, and taking walks around the neighborhood. We took him to church twice, I took him to MOPs twice, and he made road trips to Bertram twice.
Sam was an an incredibly content, easy-going, chill, happy baby. We thought Emory was an easy baby, but Sam put her to shame. He only fussed or cried if he was hungry, tired, or needed a diaper change.
I took Sam to his two month pediatrician appointment in Tyler with Dr. Hardy on November 24. It was an uneventful appointment: he was gaining weight well, he got his two month shots, and his oxygen sats were around 80, which was normal for him.
Over the next week, which included Thanksgiving and visiting lots of family, he got fussy and started spitting up. I was pumping and bottle feeding, but the only thing that really settled him was nursing. He was just not acting like himself. When we got back from Thanksgiving, I called the pediatrician to set up an appointment to talk to her about what I thought was reflux. When I took him on that Wednesday, December 3, he had only gained two ounces in a week and a half, and his sats were in the 50s and 60s. Dr. Hardy called Dr. Kao to set up an appointment for the next day. I actually considered taking Sam and the girls to the appointment by myself, but I'm so thankful now that I didn't.
Stephen and I took Sam to see Dr. Kao on December 4. Each appointment with Dr. Kao started with all the normal baby vital checks, plus a pulse ox test and an EKG. Looking back at the pictures, I can tell how blue he looked.
Sam's oxygen sats were measuring in the 50s and 60s. Dr. Kao rushed into the exam room, rushed us into the sonography room, and the sonographer, John, started doing an echo. They left the pulse ox on during the echo, and Dr. Kao was able to see what Sam's heart was doing on the echo each time his sats crashed. During the echo, his sats dropped to the 20s and 30s. John quickly finished the echo, and Dr. Kao walked us (Stephen carrying Sam and I pushing the stroller) to the congenital heart ICU. A team of nurses, RTs, and doctors were waiting for Sam. Dr. Kao said several times what a fighter Sam was each time he desatted. This led me to believe some kids must stop breathing during these spells.
Over the weekend, every time Sam got agitated when he was hungry or uncomfortable, he had tet spells (a rapid drop in oxygen saturation), but he was able to recover on his own without the help of medicine. On Saturday he had a really scary, sustained tet spell that required they start him on medicines to help heart function. I blogged about it {here}.
The doctors originally planned on scheduling Sam's Glenn for that Thursday, but he stayed so unstable that they moved it up to Tuesday, December 9. Stephen and I were woken up early that morning by the surgeon's nurse practitioner telling us they were going to do the surgery that morning. We had met with the surgeon previously, talked to Dr. Kao numerous times, and researched the surgery on our own, so we thought we were prepared for it. However, nothing can prepare you for walking your baby to the O.R., kissing him bye, and handing him over to doctors to perform a very serious surgery. I am not a highly anxious person, but I was terrified.
Dr. Mendeloff's NP came to the waiting room frequently to update us at each step of the surgery. When she came out to tell us Sam had come off the heart and lung bypass and was doing well, I was so relieved I just burst into tears. Sam recovered well after the Glenn. He came off the ventilator the next morning, and they were able to remove the pacing wires and chest drainage tubes as expected.
They moved him to the stepdown floor after a few days, and he started back on bottle feeding, but then he started running fever and tested positive for rhinovirus. He didn't tolerate feeds well. They fed him somewhat successfully through an NG tube, but he just didn't completely recover like they expected.
A week after his OHS, his fever spiked, so the nurse and NP suspected he might have an infection somewhere. His abdomen looked distended, and when I asked about it, the NP ordered an abdominal X-ray. The X-ray showed that his bowel loops were dilated, so they started him on antibiotics and held off feeds for 24 hours. Twenty-four hours turned to three days, which turned to five days, which turned to a week. The doctor suspected he had necrotizing enterocolitis (NEC), which could lead to a perforation and infection. He never presented symptoms normally. Babies with NEC usually get better or worse quickly, but Sam stayed about the same. Sam had countless X-rays, CT scans, and ultrasounds, none of which gave any specific answers. They eventually started Sam on feeds by NG tube, ND tube, and then by bottle. The cardiac attending docs consulted with a G.I. specialist, Dr. An, who suggested Sam might have a gut motility issue. Dr. An started Sam on a motility medicine that seemed to help a little, but he never returned to his pre-surgery feeding volume.
The weekend before Christmas, my parents brought the girls to see us.
I was so devastated that Sam had to spend his first Christmas in the hospital. I hated that we didn't get to have Christmas as a whole family. The hospital staff was incredible about trying to give us a good Christmas, but I almost wished we could have pretended like it was just a regular day. It was so depressing to be there any day, but especially at Christmastime.
They even had gifts for the girls!!
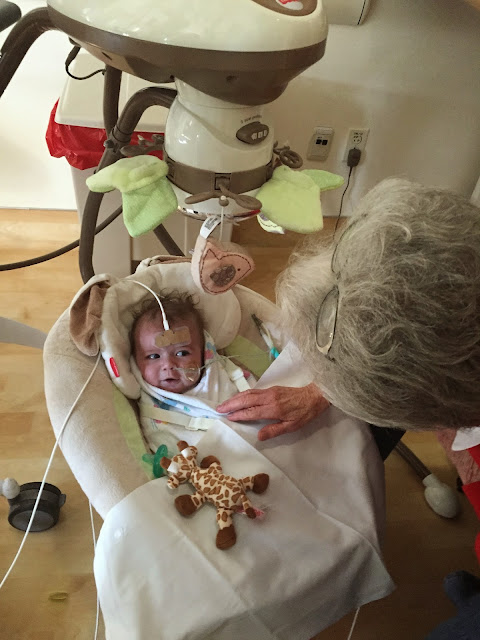
Look at that hair!
After almost a month inpatient, Sam seemed to be doing well enough. He was discharged on New Year's Day.
Continues in {Part Three}...




























.JPG)









That smile! I see so much joy in his eyes.
ReplyDelete